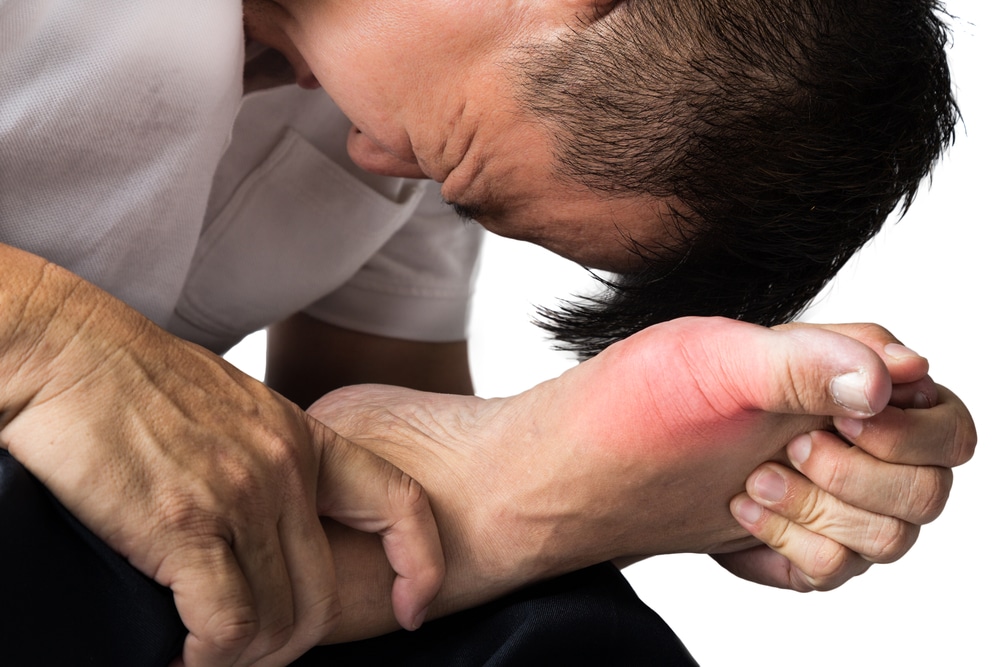
Gout is a painful form of inflammatory arthritis for which there is no known cure. But it can be managed so that it’s quite possible to live a normal life without frequently recurring gout attacks.
What is Gout?
Gout is recognized as one of the most painful types of arthritis caused by a severe inflammatory reaction to monosodium urate crystals deposited in the joints and associated soft tissue.
Often referred to in the past as “the disease of kings” or “rich man’s disease” because of their propensity to overindulge in food and alcohol, that certainly isn’t the case today…
Incidences of gout are on the increase, particularly in the West. One study in the UK showed an increase of nearly 30% between 1997 and 2012 with an estimated 1 in 40 people afflicted in 2014. A similar study in the USA, in 2011, put the number of American sufferers at 1 in 20.
It’s thought that the dramatic rise in gout over the past 20 years is due to factors such as rising obesity levels, increasing alcohol consumption, and dietary and lifestyle changes.
Symptoms
The classic symptoms of gout are:
- hot to touch
- tenderness
- taught, shiny red skin
- swelling
- inflammation
- stiffness
- severe pain
Around 70% of all gout attacks (also called “gout flares” or “gout flare-ups”) occur in the joint at the base of the big toe (the metatarsophalangeal joint) and are twice as likely to occur at night than during the daytime. But the instep, heel, side of the foot, ankle, knee, fingers, wrist, and elbow can also be targetted.
Root Cause
The root cause of gout is too-high levels of uric acid circulating in the bloodstream, a condition called hyperuricemia which, if not addressed, can lead to the formation of microscopic needle-shaped crystals of monosodium urate in the joints and surrounding tissue.
The body’s innate immune system recognizes these crystals as potentially harmful and triggers a pro-inflammatory response that floods the joint with white blood cells and inflammatory mediators to resist and eventually expel the intruders.
It’s this inflammatory response at the site that actually causes the painful symptoms we associate with gout.
What is Uric Acid?
Uric acid is the end product of purine metabolism, which purines are natural chemical compounds found in the cells of all living things, including humans, animals and plants. When cells die their purines breakdown and produce uric acid.
In a healthy body most of the uric acid produced is dissolved in the blood, filtered through the kidneys, and expelled in the urine, with a little through the stools. The rest is retained in the blood as a powerful antioxidant that can neutralize the free radicals that cause many illnesses and chronic diseases.
However, there are 2 conditions that can increase uric acid concentrations in the blood, potentially leading to hyperuricemia and gout. These are:
- the body producing too much uric acid for the kidneys to handle; called “overproduction.”
- the kidneys not filtering and excreting uric acid fast enough; referred to as “underexcretion.”
Although each can increase uric acid on its own account, underexcretion and overproduction can occur simultaneously. For example, excess alcohol consumption not only impedes uric acid excretion, it also increases uric acid production, which is why alcohol has been identified as one of the highest risk factors for gout.
Another cause of increased uric acid is too much fructose consumption…
What is Fructose?
Fructose can be found in table sugar and a whole array of processed foods and drinks often in the form of High Fructose Corn Syrup (HFCS).
Fructose can also be found naturally in some fruits and vegetables, but in lower concentrations.
When too much fructose is ingested it can raise uric acid levels in several ways:
- When fructose breaks down, lactic acid is produced. Studies have found a link between increased lactic acid and a decrease in uric acid excretion.
- Too much fructose can lead to insulin resistance which has also been linked to decreased excretion of uric acid.
- It’s been found that when the liver has to deal with too much fructose it results in elevated uric acid.
- Fructose is known to increase the breakdown of ATP (adenosine triphosphate), a molecule in the body which is the primary source of energy for the cells. It also happens to be a purine so, as it breaks down, uric acid is produced.
So too much fructose can decrease uric acid excretion and, at the same time, increase uric acid production, thus increasing the risk of hyperuricemia and gout.
And we shouldn’t forget that too much sugar can also cause weight gain which is another high risk factor for gout.
What Are Safe Levels of Uric Acid?
According to the American College of Rheumatology, the target is to have a serum uric acid level less than 6 milligrams per deciliter (6 mg/dL).
However, some people can have levels over 9.0 mg/dL and still not suffer from gout attacks. Equally, gout is found in patients with levels under 6 mg/dL.
The reasons for this aren’t known but, generally speaking, it’s agreed that a person with high uric acid is at a higher risk of gout than someone with low levels of uric acid.
Much depends on the individual but, as a general rule of thumb, maintaining your levels below 6 mg/dL is a good target.
How is Gout Diagnosed?
Your doctor will usually ask about your symptoms, when they appeared, and inspect the physical signs. Even although the symptoms could indicate gout, they’ll want to first rule out any other possible causes by asking pertinent questions and may even arrange for an x-ray.
They may also want to quiz you on any sudden change of diet (which can elevate uric acid levels) and any medications you may be taking.
They should also ask about any family history of arthritis or gout if they don’t already have that on record.
The symptoms are so classic that many doctors, in my experience, are able to diagnose the condition just with the steps above. Some may seek confirmation through a blood test to measure uric acid serum concentration. However, uric acid levels can go down during a gout attack (nobody really knows why) so a blood test may not always be reliable at this time.
They may even arrange for synovial fluid to be drawn off (needle aspiration) and examined under the microscope for evidence of crystals in the joint. This test can also help to rule out bacterial infection as a potential cause of the symptoms.
A 2014 study by the Mayo Clinic showed that, whilst a CT scan was more accurate in patients having suffered repeat attacks, the synovial fluid test was still effective in the majority of cases and actually more accurate in identifying first time gout flare-ups.
How Long Does a Gout Attack Last?
An attack of gout can last anywhere from 3 to 21 days, sometimes even longer. The average for most people could be 7 to 10 days, but a lot depends on its location in the body, how quickly it’s diagnosed, how quickly treatment is started, and the type of treatment used.
Many folks having their first gout attack, unaware that it could be gout, don’t bother seeking medical attention and treat it at home with painkillers or anti-inflammatories. For a mild case, this usually does the trick, with the attack subsiding after two or three days.
A more severe attack usually warrants attending your doctor for a diagnosis. This level of gout can last for two to three weeks with some discomfort continuing for some time after.
The affected area usually returns to normal after an attack, however, after the first gout attack, a sufferer will be at a high risk of recurring gout. The second flare-up can occur at any time, even months after the first, but subsequent attacks will usually occur with increasing frequency and severity.
In some cases, particularly where the condition hasn’t been properly addressed, these flare-ups can merge to form almost constant gout. Chronic gout such as this can result in deformities and several serious health issues, including a higher risk of death.
Who is Most at Risk of Gout?
There are quite a number of high risk factors for developing gout. People at a higher risk of gout are those that:
- are male, typically between the ages of 30 and 50 for the onset of gout.
- are female, but usually over 50 for the onset of gout (males are 10 x more likely to get gout).
- have a family history of gout or arthritis.
- are overweight.
- have a high-purine diet.
- consume too much fructose.
- drink too much alcohol.
- have certain medical conditions such as, diabetes, arteriosclerosis, hypertension, thyroid problems, and hyperlipidemia.
- have had surgery or extended bed rest.
- have had an organ transplant.
- are on certain medicines such as, diuretics, niacin (vitamin B3), salicylic acid (e.g. aspirin), levodopa, and cyclosporine.
- have had long-term exposure to lead over and above that arising from normal community exposure.
How is Gout Treated Today?
Gout is generally treated with medications: one type to help relieve the pain and inflammation and another to help lower and maintain uric acid levels. Dietary and lifestyle changes are also usually advised.
Pain and Inflammation
For pain and inflammation, non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, naproxen, indomethacin, and diclofenac can be effective.
Where a patient cannot take NSAIDs, or where they have been found to be ineffective, then colchicine may be prescribed instead. Colchicine helps to relieve pain by reducing the white blood cell count in the inflamed area.
And in the situation where a patient cannot take NSAIDs or colchicines, then corticosteroids, such as prednisone, can be prescribed. These can be administered orally or by injection into the affected area.
Uric Acid Reduction
For the reduction and maintenance of uric acid, allopurinol and the much newer febuxostat have proved effective. They come from the class of drugs called “xanthine oxidase inhibitors” which prevent the release of xanthine oxidase, which is an enzyme that aids in the breakdown of purines and the formation of uric acid.
Another common uric-acid-lowering medication is probenecid from the class of drugs called “uricosurics”. This works by increasing uric acid excretion in the urine so that uric acid levels in the blood are reduced.
Uric-acid-lowering medications have to be taken continuously as they can only work whilst being taken. In other words, if they are stopped, uric acid levels can rise again. Anyone who has been prescribed these drugs is usually advised to take them for life.
Many people find this tough to do. But if they go along the drug route they just have to, because it’s been found that stop-starting these types of medications can actually trigger gout attacks.
Diet and Lifestyle
You’ll have noticed that several of the risk factors for gout are largely controllable: being overweight, a purine-rich diet, too much fructose consumption and too much alcohol.
This is why your doctor is likely to suggest that, alongside your gout medications, you change to a low-purine diet, avoid or severely reduce your sugar/fructose and alcohol intake. And, if you’re overweight, lose those excess pounds.
Other Health Risks Associated with Gout
It’s been known for some time that frequently recurring gout can cause permanent joint damage and kidney stones. But, more recently, it’s been discovered that high uric acid can lead to many more serious health problems, even death…
A recent University of Maryland study suggested that kidney disease, kidney failure, diabetes, stroke, heart disease and increased risk of death, was linked to hyperuricemia.
In 1997, researchers at the University of Kuopio, Finland, linked high levels of uric acid to increased risk of non-fatal and fatal stroke.
In the same year, researchers at John Hopkins found that high uric acid was linked to mini strokes that, although hardly noticeable, could lead to mental decline in aging adults.
In addition, nearly 75% of gout patients exhibit metabolic syndrome, the medical term for a group of conditions associated with the development of cardiovascular disease, i.e., coronary heart disease, heart attack, congenital heart disease, angina, stroke and type 2 diabetes.
Other conditions associated with gout include:
- polycythemia (high red blood cell count)
- hemolytic anemia (high red blood cell destruction rates)
- peripheral vascular disease (poor circulation in the limbs)
- psoriasis (a chronic skin condition)
- erectile dysfunction (ED)
So, not only is it important to get rid of the excruciating pain of a gout attack, it’s absolutely vital to do everything in your power to prevent recurring gout attacks by maintaining your uric acid at healthy levels.
Living with Gout
As well as prescribing drug-based medications for your gout, your doctor is highly likely to suggest some dietary and lifestyle changes, such as:
- moving to a low-purine diet.
- avoiding/limiting fructose, HFCS, sodas/fizzy drinks, and alcohol.
- exercising regularly.
- losing excess weight.
- staying hydrated since dehydration is trigger for gout.
Remember, there’s no cure for gout. But it can be managed, so it’s possible to live a normal life, especially with an early diagnosis and adopting a healthier lifestyle.



